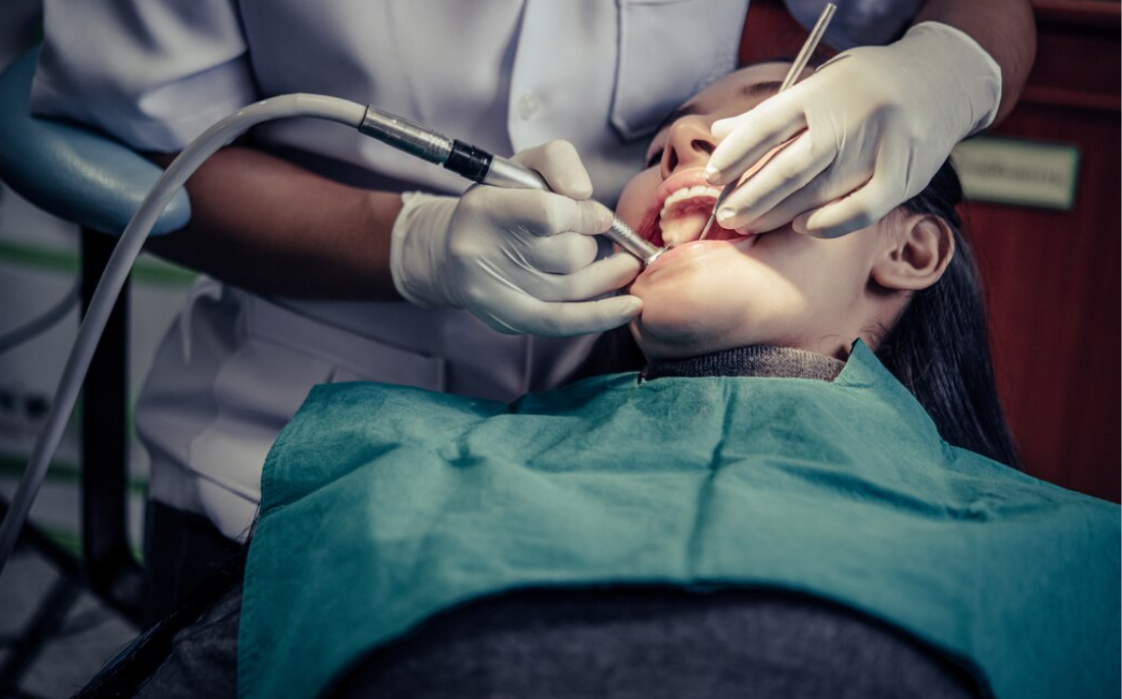
A tooth extraction is the professional removal of a tooth from its socket in the jawbone, performed by a qualified dental professional under local anaesthesia to ensure the patient is comfortable throughout the procedure. It is one of the most commonly performed dental procedures, and while it is always preferable to save a natural tooth wherever possible, there are specific clinical situations where extraction is the most appropriate and beneficial treatment for the patient’s long-term oral health. If you have been advised that a tooth needs to be removed and want honest, clear information about the process from a trusted Dental Clinic in Battersea, this comprehensive guide explains exactly how extractions work, what happens before, during, and after the procedure, and how to recover as smoothly and quickly as possible.
Tooth extractions are often surrounded by unnecessary fear and anxiety because many patients associate the procedure with significant pain or lengthy recovery. In reality, modern extraction techniques performed under effective local anaesthesia are straightforward, well-controlled procedures that most patients find considerably more comfortable than they anticipated. The discomfort experienced before the extraction, from an infected or severely damaged tooth, is almost always far greater than anything felt during or after the procedure itself. For residents seeking the highest standard of Dental Care in Battersea that prioritises patient comfort and provides clear and supportive guidance throughout every stage of the extraction process, understanding what the procedure involves removes much of the uncertainty that drives dental anxiety.
What Is a Tooth Extraction
A tooth extraction is the complete removal of a tooth from the alveolar bone, which is the specialised bone of the jaw that surrounds and supports the roots of all the teeth. The extraction releases the tooth from the periodontal ligament, which is the fibrous connective tissue that attaches the root surface to the surrounding bone, and removes the tooth from its socket entirely.
Extractions are performed as either simple or surgical procedures depending on the position, condition, and anatomy of the tooth being removed. A simple extraction is performed on a tooth that is visible above the gumline and can be accessed directly with extraction instruments. A surgical extraction is required when the tooth is not fully visible, is broken at or below the gumline, has complex root anatomy, or is impacted within the bone and requires incision of the gum and sometimes removal of a small amount of overlying bone to provide adequate access.
A qualified Dentist in Battersea who performs extractions will assess the specific tooth, review relevant X-rays, and determine which type of extraction approach is most appropriate before explaining the procedure, the anaesthesia plan, and the aftercare requirements to the patient in full.
Battersea Dental Practice is one of the best dental clinics in Battersea, providing both simple and surgical tooth extractions as part of a comprehensive range of general and specialist dental services with a genuine commitment to patient comfort and thorough aftercare support. Located at 33A Queenstown Rd, London SW8 3RE, United Kingdom, the practice is reachable at +44 20 7622 5322 or batterseadentalpractice@gmail.com to discuss concerns about a tooth that may need to be removed or to schedule an assessment appointment.
For patients who want to understand the full range of extraction and oral surgery services available, Tooth Extraction in Battersea at Battersea Dental Practice provides detailed information about the extraction procedures offered and the supportive approach taken to ensure every patient feels informed, comfortable, and well-cared for throughout their treatment.
When Is a Tooth Extraction Necessary
Preserving natural teeth is always the primary goal of quality dental care, and extraction is only recommended when it is genuinely the most appropriate clinical option for the patient’s long-term oral health. Here are the most common situations in which tooth extraction is the recommended treatment.
Severe and Irreparable Tooth Decay
When decay has destroyed so much of the tooth structure that insufficient healthy tissue remains to support a filling, crown, or other restoration, extraction becomes the most clinically appropriate response. Attempting to restore a tooth that has been compromised beyond the point of reliable repair results in a restoration that is unlikely to be durable or functional, and leaving severely decayed teeth in place risks the spread of infection to surrounding teeth and bone.
Advanced Periodontal Disease
In advanced periodontitis, the bone and connective tissue supporting the tooth are progressively destroyed by bacterial infection, causing teeth to become increasingly mobile as their supporting structures are lost. When a tooth has lost so much bone support that it cannot be stabilised through periodontal treatment and is significantly mobile, extraction is recommended to prevent the spreading infection from compromising the bone and adjacent teeth further.
Dental Infection or Abscess
A dental abscess that has spread beyond the point where root canal treatment can adequately address the infection, or a tooth with a periapical abscess that has not responded to endodontic intervention, may require extraction to eliminate the source of infection and allow the surrounding bone and tissue to heal. Untreated dental infections can spread to the jaw, neck, and in serious cases the airway, making prompt extraction an important component of infection management in severe cases.
Impacted Wisdom Teeth
Third molars, commonly known as wisdom teeth, frequently lack sufficient space to erupt into a functional position and become partially or fully impacted within the gum or bone. Impacted wisdom teeth can cause persistent pain, repeated infection of the surrounding gum tissue, damage to the adjacent second molar, and the development of cysts in the surrounding bone. Extraction is the standard treatment for problematic impacted wisdom teeth.
Orthodontic Treatment Requirements
In some orthodontic cases, one or more teeth need to be removed to create sufficient space in the dental arch for the remaining teeth to be aligned into a stable and functional position. This is most commonly required when significant crowding exists and there is insufficient room in the arch to achieve the desired alignment without creating an unstable bite or an excessively widened arch form.
Fractured Teeth Beyond Repair
A tooth that has fractured at or below the gumline, or that has developed a crack extending through the root, may be unrestorable through conventional dental treatment. When a fracture renders the tooth structurally unsaveable, extraction is the only remaining option.
Signs That a Tooth May Need to Be Extracted
There are clinical signs that indicate a tooth may require extraction rather than conservative treatment, and recognising these signs helps patients seek professional assessment promptly.
- Severe persistent toothache that does not respond to over-the-counter pain relief and has not improved over several days
- Significant swelling of the gum, cheek, or jaw around a specific tooth that may indicate a spreading infection
- A tooth that is visibly cracked, broken extensively, or so severely decayed that little healthy structure remains above the gumline
- A tooth that feels distinctly loose without any injury having occurred
- Recurrent infections or abscesses associated with the same tooth despite previous treatment
- Pain and swelling in the back of the mouth where wisdom teeth are attempting to erupt
- A tooth that your dental provider has confirmed is beyond restorative treatment after a thorough clinical and radiographic assessment
Step-by-Step: How a Tooth Extraction Works
Understanding the complete extraction process from the initial assessment through to post-operative care gives patients a clear picture of what to expect at every stage of their treatment journey.
Step 1: Pre-Extraction Assessment and Radiographic Evaluation Before any extraction is performed, the dental team conducts a thorough assessment of the tooth in question. This includes a clinical examination of the tooth and surrounding tissue, review of dental X-rays to assess root anatomy, bone levels, and proximity to anatomical structures such as the inferior alveolar nerve or the maxillary sinus, and a review of the patient’s medical history and medications. This information determines whether the extraction is suitable for the general dental setting or requires referral to an oral surgeon, and guides the anaesthesia plan and the specific extraction technique to be used.
Step 2: Medical History Review and Consent The dental team reviews the patient’s complete medical and medication history before extraction. Certain medications including blood thinners, bisphosphonates, and immunosuppressants, have direct implications for extraction safety and healing and may require coordination with the prescribing physician before proceeding. The extraction procedure, the anaesthesia plan, and the expected recovery are explained to the patient and written informed consent is obtained before treatment begins.
Step 3: Administration of Local Anaesthesia Local anaesthetic is administered to thoroughly numb the tooth, the surrounding gum, and the adjacent bone before any extraction instruments are applied. The dental team ensures that the anaesthesia is fully effective before proceeding. Most patients feel nothing more than mild pressure during the injection itself and no pain whatsoever once the area is numb. The sensation during extraction is one of pressure and movement rather than pain, and patients who experience any discomfort during the procedure should communicate this immediately so that additional anaesthetic can be administered.
Step 4: Luxation of the Tooth For a simple extraction, the dentist begins by using a dental elevator instrument to gently work between the tooth and the surrounding bone. The elevator is applied with controlled rotational and lever movements that gradually stretch and break down the periodontal ligament fibres attaching the tooth root to the surrounding alveolar bone. This process, known as luxation, progressively loosens the tooth within its socket and expands the socket to accommodate the removal of the tooth. It is the most important step in ensuring a smooth and controlled extraction.
Step 5: Tooth Removal Once the tooth has been adequately luxated, extraction forceps are applied to the tooth crown and used with controlled rocking, rotating, and pulling movements to deliver the tooth from the socket. The goal is to remove the tooth as intact as possible without leaving root fragments in the socket. For multi-rooted teeth, the roots may be removed individually if needed.
Step 6: Surgical Steps for Complex Extractions For a surgical extraction, the dentist first administers local anaesthetic and then makes a carefully planned incision in the gum tissue to create a flap that provides access to the tooth and the overlying bone. In some cases, a small amount of bone overlying the impacted or subgingival portion of the tooth is removed using a surgical handpiece to expose the tooth adequately. The tooth may be sectioned into two or more pieces using the surgical handpiece to facilitate removal in situations where the root anatomy or angulation makes intact removal difficult or inadvisable. Once the tooth is removed, the surgical site is irrigated, the bone edges are smoothed, and the gum flap is repositioned and closed with resorbable or non-resorbable sutures.
Step 7: Socket Management and Clot Formation After the tooth is removed, the socket is inspected to ensure all tooth and root material has been completely removed. Any sharp bone edges are smoothed and the socket is gently compressed to reduce its diameter. A gauze pad is placed over the socket and the patient is instructed to bite down firmly for 30 to 45 minutes to apply pressure that promotes the formation of a stable blood clot. This clot is the foundation of the healing process and its protection in the days following extraction is critically important.
Step 8: Post-Operative Instructions and Discharge Before the patient leaves the practice, detailed written and verbal aftercare instructions are provided covering what to eat and avoid, how to manage any discomfort, how to keep the extraction site clean, what activities to avoid, and what signs of potential complications to watch for. Any necessary prescriptions are provided and the next appointment is scheduled if suture removal or a follow-up assessment is required.
Simple Extraction vs Surgical Extraction: Key Differences
Understanding the distinction between these two types of extraction helps patients understand why their dental provider has recommended a specific approach and what the implications are for the procedure and recovery.
A simple extraction is appropriate for teeth that are fully visible and accessible above the gumline, have straightforward root anatomy, and can be removed intact using elevators and forceps without the need for any incision or bone removal. The procedure is typically completed in a matter of minutes per tooth once anaesthesia is established and recovery is usually uncomplicated with most patients comfortable within a few days.
A surgical extraction is required when the tooth is not fully accessible through the gum, when root anatomy is complex or divergent in a way that prevents intact removal, when the tooth is broken below the gumline, or when the tooth is impacted within the bone. Surgical extractions involve additional steps including incision, possible bone removal, and suturing, which means the procedure takes longer and recovery may involve more swelling and discomfort in the first few days than a simple extraction. However, for patients who require this approach, surgical extraction is the safest and most effective way to ensure the tooth is completely and cleanly removed without leaving root fragments or causing unnecessary trauma to the surrounding structures.
Common Patient Mistakes After Tooth Extraction
Understanding the most frequent aftercare mistakes helps patients protect their healing and avoid the complications that most commonly extend the recovery period.
Dislodging the Blood Clot Through Rinsing or Spitting: The most serious and most common post-extraction complication is dry socket, which occurs when the blood clot that forms in the extraction socket is dislodged or dissolves before the socket has healed, leaving the bone and nerve endings exposed. The most common cause of dry socket is rinsing vigorously or spitting forcefully within the first 24 hours after extraction. Patients must avoid any vigorous oral activity in the first 24 hours and rinse only very gently with warm salt water after that period.
Smoking After Extraction: Smoking is one of the leading causes of dry socket because the suction involved in smoking physically draws the blood clot out of the socket. The chemicals in tobacco smoke also interfere with wound healing and increase the risk of infection. Patients must avoid smoking for a minimum of 72 hours after extraction, with longer abstinence strongly recommended for better healing outcomes.
Eating on the Extraction Side Too Soon: Returning to normal eating habits on the extraction side of the mouth before adequate healing has occurred risks disturbing the clot and impacting food into the socket, both of which can cause pain, delay healing, and increase the risk of infection. A soft diet on the opposite side of the mouth should be maintained for at least the first three to five days following extraction.
Ignoring Worsening Pain After Day Two: Some degree of discomfort and swelling in the first two to three days after extraction is a normal part of the healing process. However, pain that is worsening rather than improving after the third day, or that is severe and unresponsive to prescribed or over-the-counter pain relief, may indicate dry socket or infection and requires prompt professional assessment rather than continued home management.
Not Completing a Course of Prescribed Antibiotics: When antibiotics are prescribed following an extraction, completing the full course as directed is essential even if symptoms improve before the medication is finished. Stopping antibiotics early allows residual bacteria to survive and potentially develop resistance, increasing the risk of a more serious and harder-to-treat post-operative infection.
Safety Considerations for Tooth Extractions
Tooth extraction is a safe and well-established dental procedure but there are important safety considerations that every patient should be aware of and discuss with their dental team before proceeding.
Patients taking anticoagulant or antiplatelet medications such as warfarin, aspirin, or clopidogrel have an increased risk of prolonged bleeding after extraction. The dental team will advise on the appropriate management of these medications before the procedure, which may involve consultation with the prescribing physician. Patients taking bisphosphonate medications for osteoporosis face a small but significant risk of osteonecrosis of the jaw following extraction and should always disclose this medication before any extraction is considered.
Patients with compromised immune systems due to medical conditions or medications, poorly controlled diabetes, or active cardiovascular disease require careful pre-extraction assessment to ensure that the procedure can be performed safely and that the post-operative healing environment is as supportive as possible.
Prevention and Aftercare Tips for Smooth Healing
The steps taken in the hours, days, and weeks following an extraction have a direct and significant impact on healing speed and the risk of complications.
- Bite firmly on the gauze pad provided for 30 to 45 minutes after the extraction to support clot formation and control initial bleeding
- Rest for the remainder of the day of extraction and avoid strenuous physical activity for at least 24 to 48 hours to prevent increased blood pressure that can disturb the clot
- Apply a cold compress to the outside of the cheek for the first 24 hours in 15-minute on and off intervals to reduce swelling
- Eat soft foods that require minimal chewing on the opposite side of the mouth for the first three to five days after extraction
- Begin gentle warm salt water rinsing 24 hours after the extraction to help keep the socket clean, rinsing two to three times daily especially after meals
- Avoid alcohol for at least 24 hours following extraction as it can interfere with healing and interact with pain medications
- Keep the head slightly elevated when lying down during the first night after extraction to reduce bleeding and swelling
- Contact the dental practice promptly if bleeding does not slow within one to two hours of applying firm pressure, if pain is worsening after day two, or if you develop fever or significant swelling
Frequently Asked Questions
- Is tooth extraction painful? The extraction procedure itself is not painful because it is performed under local anaesthetic that thoroughly numbs the tooth, surrounding gum, and bone before any instruments are applied. Patients feel pressure, movement, and vibration during the procedure but should not experience pain. Some post-operative soreness and swelling in the days following extraction is normal and expected as part of the healing process and can be effectively managed with prescribed or over-the-counter pain relief as directed by the dental team. The vast majority of patients find that the discomfort from the infected or damaged tooth before extraction is significantly greater than anything experienced during or after the procedure.
- How long does recovery from a tooth extraction take? Recovery time varies depending on the complexity of the extraction, the specific tooth involved, and the individual patient’s healing capacity. Most patients feel comfortable and are managing normal activities within three to five days of a simple extraction. Surgical extractions involving impacted wisdom teeth may cause swelling and discomfort for seven to ten days with full tissue healing occurring over the following two to four weeks. The bone within the extraction socket takes several months to fully remodel and fill in, though this process occurs gradually and does not interfere with normal function during that time.
- What is dry socket and how do I prevent it? Dry socket is a post-extraction complication that occurs when the blood clot that forms in the extraction socket is lost or dissolves before the socket has healed, leaving the underlying bone and nerve endings exposed. It presents as a worsening rather than improving toothache-like pain typically beginning two to four days after extraction, often radiating to the ear or jaw on the affected side. Preventing dry socket involves avoiding vigorous rinsing or spitting for the first 24 hours, not smoking for at least 72 hours after extraction, avoiding drinking through a straw, and eating soft foods on the opposite side of the mouth during the initial healing period. If dry socket develops, contact your dental practice promptly as it requires professional treatment to resolve.
- Do I need to replace a tooth after it has been extracted? In most cases, replacing an extracted tooth is strongly recommended to prevent the surrounding teeth from drifting into the gap over time, maintain normal chewing function, and prevent the jawbone loss that occurs in the area of a missing tooth root. The exceptions are wisdom teeth and teeth extracted specifically to create space for orthodontic treatment, where replacement is not necessary. For all other extracted teeth, replacement options including dental implants, bridges, and partial dentures should be discussed with the dental provider at or shortly after the extraction appointment.
- Can I eat normally after a tooth extraction? Normal eating should be avoided on the extraction side of the mouth for at least three to five days after the procedure. During this period, soft foods that require minimal chewing such as yogurt, mashed potatoes, scrambled eggs, soup, and smooth porridge are the most appropriate choices. Very hot foods and drinks should be avoided for the first 24 hours as heat can increase bleeding. Hard, crunchy, chewy, and spicy foods should be avoided until the extraction site has healed sufficiently to withstand normal food contact. Your dental provider will give you specific guidance on dietary restrictions based on the complexity of your individual extraction.
Conclusion
Understanding how tooth extractions work removes the fear and uncertainty that often surrounds this common and well-established dental procedure, replacing anxiety with the knowledge that modern extraction techniques are safe, comfortable, and associated with recovery periods that are far shorter and more manageable than most patients anticipate. Following pre and post-operative guidance carefully, avoiding the common aftercare mistakes that cause complications, and planning for tooth replacement where appropriate are the three steps that ensure the best possible outcome from any extraction procedure. Battersea Dental Practice, located at 33A Queenstown Rd, London SW8 3RE, United Kingdom, is one of the most trusted dental clinics in Battersea, providing expert extraction services and comprehensive aftercare support to every patient who needs this treatment. To discuss your situation or book an assessment, contact the team at batterseadentalpractice@gmail.com or call +44 20 7622 5322.